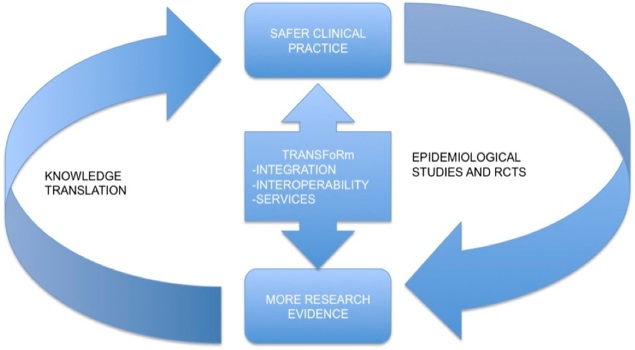
TRANSFoRm aims to develop the technology that facilitates a learning healthcare system (see Figure 1). TRANSFoRm brings together a highly multidisciplinary consortium where three carefully chosen clinical ‘use cases’ will drive, evaluate and validate the approach to the ICT challenges. The project will build on existing work at international level in clinical trial information models (BRIDG and PCROM), service-based approaches to semantic interoperability and data standards (ISO11179 and controlled vocabulary), data discovery, machine learning and electronic health records based on open standards (openEHR).
TRANSFoRm will extend this work to interact with individual eHR systems as well as operate within the consultation itself providing both diagnostic support and support for the identification and follow up of subjects for research. The approach to system design will be modular and standards-based, providing services via a distributed architecture, and will be tightly linked with the user community. Four years of development and testing will end with a fifth year that will be dedicated to summative validation of the project deliverables in the Primary Care setting.
The underlying concept of TRANSFoRm is to develop a ‘rapid learning healthcare system’ driven by advanced computational infrastructure that can improve both patient safety and the conduct and volume of clinical research in Europe.
The EU policy framework for information society and media, i2010 identifies eHealth as one of the principal areas where advances in ICT can create better quality of life for Europe’s citizens. ICT has important roles in communication, decision-making, monitoring and learning in the healthcare setting. TRANSFoRm recognises the need to advance the underpinning information and computer science to address these issues in a European and international context.
Providing interoperability between different clinical systems, across national boundaries, and integration of clinical systems and research systems lies at the heart of the eHealth Action Plan 2004. This is however, a two-way street, just as clinical data are needed for research (for participant identification and evaluation of outcomes) research data is needed to support clinical care. In both domains fragmentation of records and proprietary systems that do not adhere to standards within the domain are as much of a challenge as the legal and ethical issues that complicate access to clinical data for researchers. However, significant advances in international standards and in computational technology to support interoperability offer a way to overcome these challenges. Furthermore, advances in the understanding of clinical judgment and decision making, and the possible ways of supporting them via ICT can inform the design of more ‘intelligent’ electronic health record systems.
The single richest source of routine healthcare data lies within the records of Europe’s General Practitioners. Primary Care is responsible for first contact, continuing, and generalist care of the entire population from birth to death. Any project that aims to comprehensively support the integration of clinical and research data should begin with Primary Care. In addition, even in countries where General Practitioners do not fulfil a ‘gatekeeper’ function, controlling access to specialist services, the quality of initial diagnosis at Primary Care level determines much of the future course for an individual patient with a health problem. In order to support patient safety in both clinical and research settings, significant ICT challenges need to be overcome in the areas of interoperability, common standards for data integration, data presentation, recording, scalability, and security.
Project Brochures
Project Details
Date: 1st March 2010 to 31 May 2015
FP7 Reference: 247787
Total cost: €9,726,688
EU Contribution: €7,540,000
Sub-Programme: ICT-2009.5.2 ICT for Patient Safety